Researchers from University of Nottingham have developed software that helps predict the risk of blindness and amputation in people living with type 1 or type 2 diabetes. A free online tool is available and it takes less than a minute to get results.
People with diabetes who are at high risk of blindness and amputation because of their condition could get better preventative treatment thanks to two new risk prediction tools created by University of Nottingham researchers and medical software company Clinrisk Ltd.
The tools use existing patient data and will help to personalise care and advice and to target resources at those in greatest need. They are based on information that patients are likely to know, or that is routinely recorded in general practice computer systems. The study is published in The BMJ this week.
A link to the online version of the tool can be found later in this article.
Patients with type 1 or type 2 diabetes are at increased risk of blindness and amputation. Diabetic eye disease is now the second most common cause of blindness in people of working age in the United Kingdom, while more than 7,000 diabetes related amputations take place annually in England.
Continue Reading Below ↓↓↓
Despite the frequency of these complications and their effect on patients, methods of identifying those at greatest risk are lacking.
Professor Julia Hippisley-Cox and Professor Carol Coupland at The University of Nottingham set out to develop and validate a new risk prediction algorithm to predict the absolute risk of developing these complications over a 10 year period in men and women with diabetes.
The team used anonymised patient data derived from the QResearch database – a not-for-profit partnership between The University of Nottingham and leading healthcare technology provider EMIS. The analysis is based on around 455,000 people with diabetes aged 25-84 years from 763 general practices in England.
Individual risk factors that could influence the results, such as ethnicity, smoking, body mass index, blood pressure and cholesterol levels were taken into account.
Mathematical models were then used to calculate separate risk equations for the 10 year risk of blindness and amputation.
Data from a further 254 QResearch practices and 357 general practices from the Clinical Practice Research Datalink were used to validate the two models, which performed well, explaining around 41 per cent and 32 per cent of the variation in time to amputation and blindness, respectively in men and 38 per cent and 31 per cent respectively in women.
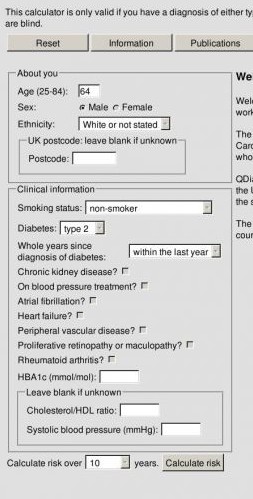
The researchers also developed a web-based calculator so that clinicians can enter their patients’ data, and patients can enter their own data, to determine the 10 year risk of these complications.
Professor Hippisley-Cox said: “To our knowledge, these are the first tools for predicting the 10 year risk of both blindness and amputation, two of the complications that most concern patients with diabetes and affect quality of life. We have some study weaknesses, including the lack of formal adjudication of diagnoses and the potential for bias due to missing data. But more accurate individualised information on the risk of complications may help patients to make more informed decisions about the balance of risks and benefits of treatment options reflecting their own values and choices.”
The study concludes that, for clinicians and the health service, more accurate methods for stratifying patients according to their absolute risk of complications could enable screening programmes to be tailored to an individual’s level of risk and support the more rational use of scarce resources.
In an accompanying editorial in The BMJ, Professor Azeem Majeed and Mariam Molokhia say the new risk prediction models “can help to provide the basis of a more individualised and holistic method of tackling these complications in patients.”
Continue Reading Below ↓↓↓
They point out the need to test the models in actual practice – and to test their impact outside the UK, particularly in countries with the highest prevalence of diabetes.
However, they say the tools “are one example of the value of the data held by the NHS in its electronic medical records and administrative databases.” These data “have great potential to improve NHS clinical care as well as giving patients information to help them make better decisions about their own health.”
Use the web calculator right now using this link: Calculate the absolute risk of complications among patients with diabetes.
Source: University of Nottingham
Journal: The BMJ