NORTH CHICAGO, ILL. -- Transplantation of insulin-producing pancreatic beta-cells shows great promise as a treatment for type 1 diabetes, but development of this therapy has been hampered by a severe shortage of donor beta-cells, which are obtained from deceased human donors. In research published in the October issue of Nature Biotechnology, Ji-Won Yoon, PhD, Professor of Pathology and Director of the Rosalind Franklin Comprehensive Diabetes Center at Rosalind Franklin University of Medicine and Science, Dr. Naoya Kobayashi (Okayama University Graduate School of Medicine and Dentistry), and their international colleagues describe a "reversibly immortalized" cell line that can supply large amounts of insulin-producing human beta-cells. Ultimately, a cell line of this sort may provide an abundant source of beta-cells for transplantation and an alternative to beta-cells from cadavers.
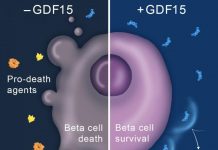
Type 1 diabetes results from the loss of insulin-producing beta-cells in the pancreas. Because the supply of beta-cells from cadavers is insufficient to meet the needs of 99% of diabetic patients, alternative sources of beta-cells would be highly desirable. Previous efforts to coax mature human beta-cells to survive and replicate in the laboratory have not succeeded, however, because the cells died or lost their ability to produce insulin in response to sugar stimulation.
Dr. Yoon, Dr. Kobayashi and colleagues got around this problem by manipulating and analyzing large numbers of human beta-cells. First, they added genes that extend cell lifespan to human beta-cells and looked for the rare cells that did not form tumors and that expressed insulin or other beta-cell proteins. Out of more than 250 cells lines screened, only one passed this test. This cell line was allowed to replicate to produce large numbers of cells. Then, the genes that extend cell lifespan were removed to ensure that the cells would not form tumors and to promote beta-cell behavior. The resulting cells produced about 40% as much insulin as normal beta-cells and successfully controlled blood sugar levels in diabetic mice for more than 30 weeks.
While further research is needed before these cells can be considered for testing in humans, plans to develop a "universal beta-cell line" are well underway, and Dr. Yoon anticipates that human clinical trials might begin as soon as three to five years from now. The discovery of this technique to create a reversibly immortalized beta-cell line represents a significant leap in the quest to develop an effective and universal treatment for type 1 diabetes; it is estimated that 18.2 million Americans suffer from diabetes. The long-term impact of this discovery, and those that will follow, will undoubtedly be profound and far-reaching.
Rosalind Franklin University of Medicine and Science educates medical doctors, health professionals and biomedical scientists in a personalized atmosphere. The University is located at 3333 Green Bay Road, North Chicago, IL 60064, and encompasses Chicago Medical School, College of Health Professions, Dr. William M. Scholl College of Podiatric Medicine, and School of Graduate and Postdoctoral Studies. Visit at www.rosalindfranklin.edu.
Continue Reading Below ↓↓↓
Source: Rosalind Franklin University of Medicine and Science