November 2005 -- Researchers are using a new cell transplantation technique to restore the cells that produce insulin in patients with type 1 diabetes. The method is minimally invasive, with few complications. The study was presented at the annual meeting of the Radiological Society of North America (RSNA).
"We used ultrasound guidance to inject donor cells into the portal vein of diabetic patients, which is accessed through the skin," said co-author Saravanan Krishnamoorthy, M.D., radiology resident at the University of Minnesota in Minneapolis. "This is a safe method of cell transplantation that could potentially become a same-day procedure."
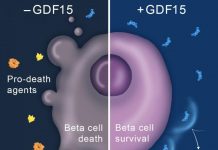
In type 1 diabetes, the body does not produce insulin. This typically results from the destruction of insulin-producing islet beta cells in the pancreas. Insulin is necessary to metabolize sugar, which is the basic fuel that all cells need.
With this minimally invasive technique, donor islet cells are injected into diabetic patients so that the new, healthy islet cells can restore insulin production, essentially stopping the progression of the disease. The study included 13 patients with poorly controlled type 1 diabetes. Fifteen islet cell transplants were completed-two patients underwent two procedures to achieve correct needle placement.
"We used a steroid-free protocol to suppress the immune system, so that the body accepted the transplanted cells," Dr. Krishnamoorthy said. "We also developed a 'sandwich technique' to close the access site through the skin, where the islet cells are injected. The sandwich technique is so-called because of the layered applications of gelfoam and coil used to close the access site."
Continue Reading Below ↓↓↓
Dr. Krishnamoorthy said that even though percutaneous islet cell transplantation is currently an experimental procedure, the sandwich closure is a safe method that prevents many of the complications common to previous techniques used to transplant islet cells. Thirty days after the procedure, all 13 patients were producing insulin without requiring supplemental injections, and none experienced major complications. Liver function tests and blood cell counts were monitored carefully during this time.
In the future, Dr. Krishnamoorthy looks toward the potential use of stem cells for this purpose, and also the development of better immunosuppressive medications to keep the body from rejecting the transplanted islet cells.
Type 1 diabetes, formerly known as juvenile diabetes, is a debilitating disease that is usually diagnosed in children and young adults. It can result in significant morbidity, causing vision loss, loss of sensation that results in severe infections, fractures and amputations, destruction of major organ function (e.g., the kidneys) and cardiovascular disease that can result in complications such as heart attacks. Both genetic and environmental factors contribute to the disease.
Source: RSNA