Scientists were able to reduce healing time for skin ulcers and bedsores by a third, as well as reduce the chance of wound infection, by using low-intensity ultrasound. Treatment was especially effective in people with diabetes.
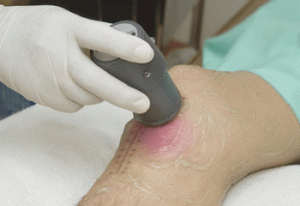
Healing times for skin ulcers and bedsores can be reduced by a third with the use of low-intensity ultrasound, scientists from the University of Sheffield and University of Bristol have found.
Researchers from the University of Sheffield’s Department of Biomedical Science discovered the ultrasound transmits a vibration through the skin and wakes up cells in wounds helping to stimulate and accelerate the healing process.
More than 200,000 patients in the UK suffer with chronic wounds every year at a cost of over £3.1 billion to the NHS.
Continue Reading Below ↓↓↓
The ultrasound treatment, which also reduces the chance of wounds getting infected, is particularly effective when treating diabetics and the elderly.
There are 11 million over-65s, three million diabetics, and 10 million smokers in the UK – all of whom are likely to suffer problems with healing wounds.
A quarter of diabetics suffer from skin ulcers, particularly foot ulcers, due to the loss of sensation and circulation in the legs.
Lead author of the study Dr Mark Bass, from the University’s Centre for Membrane Interactions and Dynamics (CMIAD), said: “Skin ulcers are excruciatingly painful for patients and in many cases can only be resolved by amputation of the limb.
“Using ultrasound wakes up the cells and stimulates a normal healing process. Because it is just speeding up the normal processes, the treatment doesn’t carry the risk of side effects that are often associated with drug treatments.”
The pioneering study, which is published in the Journal of Investigative Dermatology, was carried out in collaboration with the School of Biochemistry at the University of Bristol, the Wound Biology Group at the Cardiff Institute of Tissue Engineering and Repair, and the orthopaedic company, Bioventus LLC.
Dr Bass added: “Now that we have proven the effectiveness of ultrasound we need to explore the signal further. We have found that the ultrasound signal we currently use is effective, but it is possible that by refining the treatment we could improve the effects even further. “Because ultrasound is relatively risk free we could expect to see it in broad clinical use within three or four years.”
Source: University of Sheffield
Journal: Journal of Investigative Dermatology









