New study finds that a protein that normally fosters tissue repair instead acts to inhibit healing when sugar levels are high. The role reversal helps explain why wounds heal slowly in people with diabetes.
For diabetes patients, even a cut or scrape can result in severe complications. Because the skin doesn’t close promptly, bacteria can get a foothold in the injured tissue, leading to chronic ulcers that in some cases require amputations.
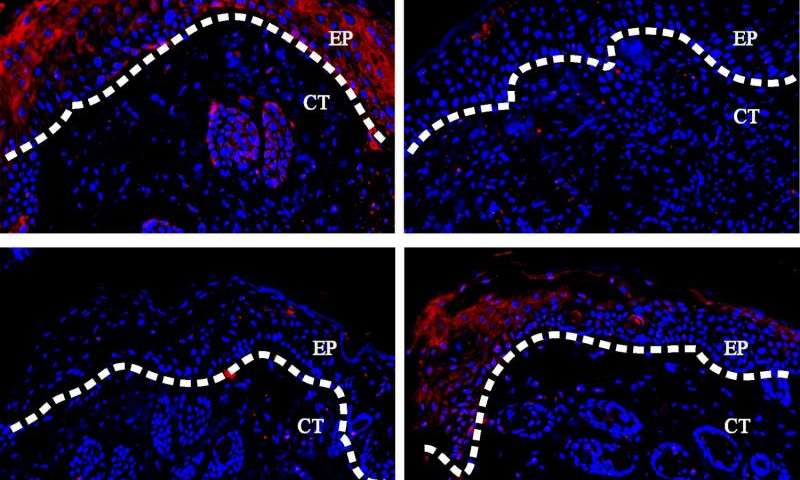
In a previous study, Dana Graves and colleagues from the University of Pennsylvania School of Dental Medicine found that the protein FOXO1 orchestrates an important early step in healing by promoting the skin cells known as keratinocytes to migrate into the injury, thus building an epithelial layer to cover the wound.
FOXO1 spurs their movement by binding to the promoter of TGFB1, a gene that encodes transforming growth factor beta 1 (TGF-β1), a protein that triggers pro-healing responses. FOXO1 levels rise in wounds of diabetic mice, but nobody had determined whether the high sugar levels in these animals alter the protein’s function during healing.
To answer this question, Graves and colleagues compared the healing capabilities of control mice and mice that lack FOXO1 in their keratinocytes. In animals with normal blood sugar, small skin wounds mended more slowly in the absence of FOXO1. But in mice that had diabetes, wounds healed faster if FOXO1 was missing. Seven days after diabetic animals were injured, the wounds were mostly closed in the animals lacking FOXO1 but remained mostly open in the group that still produced FOXO1.
Graves and colleagues discovered that, in the presence of high glucose levels, FOXO1 slows keratinocyte migration. They determined that sugar changes FOXO1’s relationship with TGF-β. At normal sugar levels, cultured keratinocytes produced 45% less TGF-β if they were missing FOXO1.
Continue Reading Below ↓↓↓
But at high sugar concentrations, cells’ FOXO1 status had no impact on their TGF-β production, suggesting that FOXO1 no longer regulates TGF-β under these conditions. High sugar levels prevented FOXO1 from binding to the TGFB1 promoter, the researchers found. Instead, FOXO1 turns on two genes that curb keratinocyte migration and block wound healing when expressed at high levels.
People with diabetes often produce too little insulin, and the researchers showed that the hormone counteracts FOXO1. For example, high glucose levels boost production of FOXO1, but the researchers found that insulin reversed this effect. The hormone also sped up migration of keratinocytes cultured in high-sugar conditions.
Two other metabolic malfunctions common in diabetes patients also impede wound healing through FOXO1, the researchers discovered. As blood sugar levels rise, glucose can glom onto proteins and alter their functions.
The team found that one glucose-modified protein prevented FOXO1 from attaching to TGFB1’s promoter, thereby slowing keratinocyte movement. Moreover, levels of the inflammation-promoting molecule TNFα are often high in diabetics. The researchers determined that TNFα similarly blocked FOXO1’s interaction with the TGFB1 promoter and inhibited keratinocyte migration.
“Whether FOXO1 is beneficial or harmful, whether it promotes healing or inhibits healing, depends on the environment of the cell,” says Graves.
Previous studies showed that insulin stimulates wound healing in diabetics. These findings support further tests of this potential treatment and suggest that inhibiting FOXO1 could speed healing in patients with diabetes.
Citation: Zhang, C., et al. 2015. J. Cell Biol. doi:10.1083/jcb.201409032
Source: Rockefeller University Press
Journal: Journal of Cell Biology