Findings from Boston University School of Medicine (BUSM), which appear in eLife, provide a possible explanation as to why most people who are obese develop insulin resistance and type 2 diabetes.
A minority of obese individuals, the so-called healthy obese, have normal insulin sensitivity and are not diabetic.
The BUSM researchers have been studying a protein called PTRF (Cavin-1) whose absence in model organisms and humans results in a nearly complete loss of fat cells, a condition called lipodystrophy.
According to lead author Libin Liu, PhD, Instructor of Biochemistry, and Paul Pilch, PhD, Professor of Biochemistry and Medicine at BUSM, this lack of fat cells causes fat to be mis-targeted to other tissues where it causes them to become insulin resistant. Eventually type 2 diabetes develops.
Paradoxically, most obese individuals have an abundance of fat cells but they develop insulin resistance and their fat is also mis-targeting to other tissues.
Continue Reading Below ↓↓↓
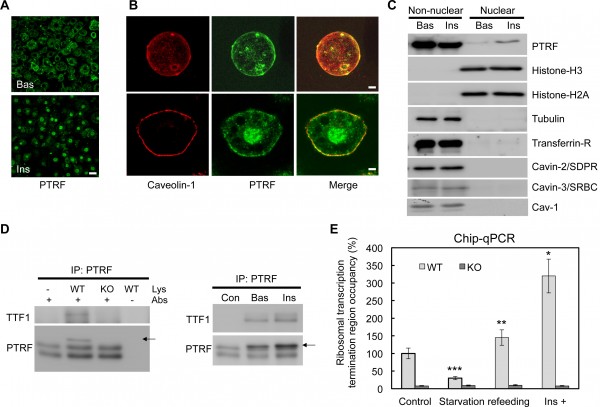
Liu and Pilch analyzed normal model organisms and compared them to those lacking PTRF. They also studied fat cells grown in the lab that either had PTRF or lacked it. Cells need to respond to rapid nutritional challenges by making new proteins to efficiently store fat.
These challenges correspond to those of the nutrient-rich diet common in Western society, and increasingly, worldwide. In the absence of PTRF, cells were unable to make sufficient new protein to respond adequately to cycles of fasting and refeeding, the equivalent of the human dietary cycle.
Further studies described how PTRF works at the molecular level, and the inefficiency of this process in most instances of obesity may be the link between the similar deleterious consequences of too little and too much fat.
Describing the role of PTRF and gaining a better understanding of how fat can be distributed in these models may eventually offer new opportunities to treat diabetes in humans.
The authors caution, however, that type 2 diabetes is a complex condition and proteins other than PTRF can also contribute to the development of the disease.
Even as more research unfolds, Liu and Pilch add: “Diet and exercise continue to be the first choice for preventing and treating Type 2 diabetes.”
The study was funded by a National Institutes of Health grant, DK097708.
Source: Boston University Medical Center
Journal: eLife
Funder: National Institutes of Health
Related Journal Article: PTRF/Cavin-1 promotes efficient ribosomal RNA transcription in response to metabolic challenges
Image courtesy of eLife (CC)