The FDA has issued a statement about their review of the affect the blood-thinning drug Plavix has on the risk of death in patients with heart disease, or at risk for heart disease.

A U.S. Food and Drug Administration (FDA) review has determined that long-term use of the blood-thinning drug Plavix (clopidogrel) does not increase or decrease overall risk of death in patients with, or at risk for, heart disease.
Their evaluation of the Dual Antiplatelet Therapy (DAPT)1 trial and several other clinical trials also does not suggest that clopidogrel increases the risk of cancer or death from cancer.
Patients should not stop taking clopidogrel or other antiplatelet medicines because doing so may result in an increased risk of heart attacks and blood clots. Talk with your health care professional if you have any questions or concerns about clopidogrel. Health care professionals should consider the benefits and risks of available antiplatelet medicines before starting treatment.
Clopidogrel is an antiplatelet medicine used to prevent blood clots in patients who have had a heart attack, stroke, or problems with the circulation in the arms and legs. It works by helping to keep the platelets in the blood from sticking together and forming clots that can occur with certain medical conditions.
Continue Reading Below ↓↓↓
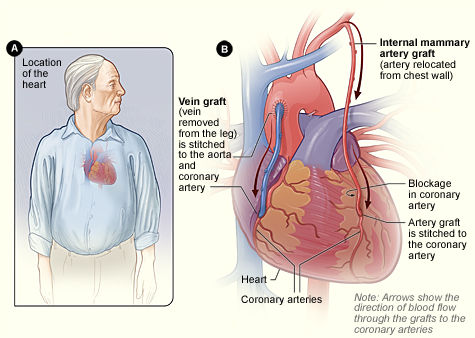
Results from the DAPT trial were published in the New England Journal of Medicine in November 2014. The DAPT trial compared treatment with dual antiplatelet therapy (either clopidogrel [Plavix] or prasugrel [Effient] plus aspirin) for 12 months versus 30 months in patients who had undergone placement of a drug-eluting coronary stent. Compared to patients taking clopidogrel for 12 months, patients who were treated with clopidogrel for 30 months had lower rates of heart attacks and stent thrombosis but higher rates of death, primarily from cancer or trauma.
In order to investigate the increased risk of death and cancer-related death reported with clopidogrel in the DAPT trial, FDA examined the results of the DAPT trial and other large, long-term clinical trials of clopidogrel with data available on rates of death, death from cancer, or cancer reported as an adverse event.2-13
FDA performed meta-analyses of other long-term clinical trials to assess the effects of clopidogrel on death rates from all causes. The results indicate that long-term (12 months or longer) dual antiplatelet therapy with clopidogrel and aspirin do not appear to change the overall risk of death when compared to short-term (6 months or less) clopidogrel and aspirin, or aspirin alone. Also, there was no apparent increase in the risks of cancer-related deaths or cancer-related adverse events with long-term treatment.
The following table shows the results from the meta-analyses:
| Number of patients included | Long-term clopidogrel plus aspirin | Short term clopidogrel plus aspirin or aspirin alone | |
|---|---|---|---|
| Overall incidence of death | 56,799 | 6.7% | 6.6% |
| Incidence of cancer adverse events | 37,835 | 4.2% | 4.0% |
| Incidence of cancer death | 40,855 | 0.9% | 1.1% |
Additional Information for Patients and Caregivers
- Based on our reviews of the Dual Antiplatelet Therapy (DAPT) trial and several other large clinical trials, we have concluded that treatment with clopidogrel does not appear to change the overall risk of death in patients with, or at risk for, coronary artery disease.
- Clopidogrel is an antiplatelet blood-thinning medicine that may help prevent future heart attacks, strokes, and other clot-related diseases in patients who have already had a heart attack, stroke, or have certain cardiovascular conditions.
- Do not stop taking clopidogrel without first talking to your health care professional. Suddenly stopping the use of antiplatelet medicines can put you at risk for heart attacks, strokes, and blood clots.
Be aware that while taking clopidogrel you may bruise more easily, and it may take longer for any bleeding to stop. - Discuss any questions or concerns about clopidogrel with your health care professional.
Read the patient Medication Guide you get along with your clopidogrel prescriptions. It explains the benefits and risks associated with the use of clopidogrel. - Report any side effects you experience to your health care professional and the FDA MedWatch program.
Additional Information for Health Care Professionals
- Based on our reviews of the Dual Antiplatelet Therapy (DAPT) trial and several other large, long-term clinical trials, we have concluded that there is no evidence of either a harmful or beneficial effect of clopidogrel on all-cause mortality or cancer-related deaths in a population with, or at risk for, coronary artery disease. That is, the adverse mortality findings in the DAPT trial were not confirmed.
- Clopidogrel is approved for use in combination with aspirin in patients with acute coronary syndrome, or in patients not on aspirin with a history of recent myocardial infarction, recent stroke, or established peripheral arterial disease.
- When selecting antiplatelet therapy for patients with an acute coronary syndrome who are managed with coronary stent implantation, prescribers should consider that prasugrel and ticagrelor have been shown to be superior to clopidogrel when used in this patient population. In addition, in patients with a history of myocardial infarction one to three years prior to study enrollment, ticagrelor has also been shown to reduce the risk of cardiovascular death, myocardial infarction, and stroke.
- We are working with the manufacturers of clopidogrel to update the label to reflect the results of the mortality meta-analysis.
- Inform patients about the increased risk of bleeding and bruising when taking clopidogrel.
- Advise patients to report any unanticipated, prolonged, or excessive bleeding, or blood in their stools or urine.
- Encourage patients and caregivers to read the patient Medication Guide they received with clopidogrel prescriptions.
- Report any side effects you experience to your health care professional and the FDA MedWatch program.
References:
- Mauri L, Kereiakes DJ, Yeh RW, et al. Twelve or 30 months of dual antiplatelet therapy after drug-eluting stents. N Eng J Med 2014;371:2155-2166.
- Connolly SJ, Yusuf S, Budaj A, et al. Rationale and design of ACTIVE: the Atrial Fibrillation Clopidogrel Trial with Irbesartan for Prevention of Vascular Events. Am Heart J 2006;151:1187-1193.
- Berger JS, Bhatt DL, Steg PG, et al. Bleeding, mortality, and antiplatelet therapy: results from the Clopidogrel for High Atherothrombotic Risk and Ischemic Stabilization, Management, and Avoidance (CHARISMA) trial. Am Heart J 2011 Jul;162(1):98-105.
- Yusuf S, Zhao F, Mehta SR, et al. Effects of clopidogrel in addition to aspirin in patients with acute coronary syndromes without ST-segment elevation (CURE trial). N Engl J Med 2001 Aug 16; 345(7):494-502.
- Steinhubl SR, Berger PB, Mann JT 3rd, et al. Clopidogrel for the Reduction of Events During Observation (CREDO): early and sustained dual oral antiplatelet therapy following percutaneous coronary intervention: a randomized controlled trial. JAMA 2002 Nov 20;288(19):2411-20.
- The SPS3 Investigators. Effects of clopidogrel added to aspirin in patients with recent lacunar stroke. N Engl J Med 2012 Aug 30;367:817-825.
- Lee CW, Ahn JM, Park DW, et al. Optimal duration of dual antiplatelet therapy after drug-eluting stent implantation: a randomized, controlled trial (DES-LATE). Circulation 2014 Jan 21;129(3):304-312.
- Belch JJ, Dormandy J, CASPAR Writing Committee, et al. Results of the randomized, placebo-controlled clopidogrel and acetylsalicylic acid in bypass surgery for peripheral arterial disease (CASPAR) trial. J Vasc Surg 2010 Oct;52(4):825-833.
- Valgimigli M, Camp G, Monti M, et al. Short- versus long-term duration of dual-antiplatelet therapy after coronary stenting: a randomized multicenter trial (PRODIGY). Circulation 2012 Apr 24;125(16):2015-2026.
- Colombo A, Chieffo A, Frasheri A, et al. Second-generation drug-eluting stent implantation followed by 6- versus 12-month dual antiplatelet therapy: the SECURITY randomized clinical trial. J Am Coll Cardiol 2014 Nov 18-25;64(20):2086-2097.
- Feres F, Costa RA, Abizaid A, et al. Three vs twelve months of dual antiplatelet therapy after zotarolimus-eluting stents: the OPTIMIZE randomized trial. JAMA 2013 Dec 18;310(23):2510-2522.
- Park KW, Chae IH, Lim DS, et al. Everolimus-eluting versus sirolimus-eluting stents in patients undergoing percutaneous coronary intervention: the EXCELLENT (Efficacy of Xience/Promus Versus Cypher to Reduce Late Loss After Stenting) randomized trial. J Am Coll Cardiol 2011;58(18):1844-1854.
- Kim BK, Hong MK, Shin DH, et al. A new strategy for discontinuation of dual antiplatelet therapy: the RESET Trial (Real Safety and Efficacy of 3-month dual antiplatelet Therapy following Endeavor zotarolimus-eluting stent implantation). J Am Coll Cardiol 2012 Oct 9;60(15):1340-1348.
Source: FDA